3. Pain management
25. Opioid therapy in addicted patients: background and perspective from the UK
William Notcutt
Three Casesa
Case 1
Alesha, age 35, has chronic leg pain secondary to vascular damage from previous recurrent groin infections associated with intravenous opioid use. Having a baby was the stimulus to come off her drugs but she has struggled to maintain this state because of her pain and her impoverished living conditions. She sometimes smokes cannabis to relax and help her sleep. She uses codeine, which is of minimal help for the pain. She is supported by a psychiatric social worker who attends the clinic with her and she has never missed an appointment. These are now at 3-month intervals. She does not get on with her GP who she describes as an “Arse.”
Should she be prescribed a long-acting opioid, such as slow release morphine, in a dose that will give her reasonable control?
Case 2
Ian, age 54, has been admitted to hospital with acute alcohol poisoning. He drinks two to three bottles of spirits a day. He also takes morphine for chronic back pain due to two wedge fractures of lumbar vertebra. He has been with the addiction services in the past, but has a chaotic lifestyle. His GP provides him with oral morphine for his pain. He only likes immediate release opiates, but has remained on a stable dose for some months. On the acute medical ward he is suffering severe withdrawal symptoms and has been given chlordiazepoxide. He has not had morphine for 2–3 days.
Should he have his morphine restarted at the previous dose?
Case 3
Peter, age 40, has had three prison terms for violence. He has a significant history of drug misuse. He has chronic low back pain for 12 years and has been through a full range of investigation and therapy. He is using slow release morphine, diazepam, and amitriptyline. When he can get cannabis, he finds this is very effective for symptom control. He says that his back is much worse now and asks for an increase in opiate. He indicates that he might go back to buying on the street.
Should the physician increase his morphine dose, or prescribe him a synthetic cannabis analogue?
Most, if not all, doctors and nurses in the UK are now educated in the basics of ethics and are familiar with the common four principles of autonomy, beneficence, nonmaleficence, and justice/fairness. They are easy to understand and to apply to clinical practice as a source of guidance. Further, there is a perception in the UK that a court would look favorably on a doctor who has acted using reasonable and demonstrable ethical process in decision-making, whatever the outcome (based on the UK tradition of the Bolam Test1 and later, the Bolitho judgment,2 in determining negligence).3
Ethical principles
Autonomy
Just because a patient has a dependency problem, this is no justification for denying their right to have their pain managed in an appropriate fashion and to being involved in decisions about treatment. Pain control may be difficult to achieve but clinicians have a duty of care to attempt this. The patient should have some autonomy to determine, within reason, his or her preferred approach. In cancer care we allow the patient to decide on treatment, from a range of drug and procedure options that may all be potentially toxic and harmful. Equally, we don’t agree to harmful therapeutic options. Doctors and nurses also have the right to not being abused, either by the patient, relatives, friends, or by the state authorities.
Beneficence
There is a widely held acceptance that pain control has benefits for both the individual and those around him/her. Therefore, beneficence is achieved by working towards this goal. However, determining the balance between analgesia and feel-good/pleasure effects in a patient with a significant dependency potential is difficult. A patient is likely to derive health benefits from having a prescribed, standardized, and uncontaminated source of their drug rather than being tempted to purchase on the street. Working with others to control abnormal behaviors associated with pain and to reduce chaotic lifestyles will be helpful, although for some patients this may become mere containment of the situation rather than progressive improvement. Containment, however, is better than deterioration.
Nonmaleficence
Providing a legitimate source of a drug for pain has its risks. A patient may see this as a way to support a drug dependency habit if the doctor can be convinced that the pain is the dominant problem. However, failing to help a patient with chronic pain may have a major impact on the rest of the family and local society. A similar situation occurs when such a patient is admitted to a ward with an acute pain problem. They can be disruptive when they cannot get their usual level of drug intake, or the extra medication, or alternatives needed to control the additional pain. One common reason for failure to manage this situation is that the doctors lack knowledge in prescribing appropriate amounts of medication. For example, finding patients prescribed a mere 10 mg of oral morphine for breakthrough pain, when their normal daily baseline intake is 500 mg of morphine, is a common occurrence. Similarly, wholly inadequate bolus doses of opioid are often programmed into PCA devices for post-operative pain in these patients, because doctors are terrified of causing an overdose by giving more than the standard dose used for an opioid naïve patient. Lack of adequate education in pain management for all clinicians is a serious systemic ethical failure.
Inevitably there are the occasional tragedies, as opioids are dangerous in the wrong hands. A patient of the author’s, who had proved very difficult to manage, went for a night out with a friend. While away, the troubled adolescent daughter broke into her mother’s apartment with some friends and decided to have a party. She searched out her mother’s slow-release morphine for a “trip,” vomited while unconscious, and died. While these occurrences should lead to a search for safeguards, they are not an adequate excuse for not providing, or attempting to provide, appropriate analgesia for pain.
Justice
Perhaps the most common ethical principle that is flouted is that of justice and fairness. Patients with dependency problems are often given a low priority for pain therapy due to their drug habit, lifestyle, attitudes to staff, and other personal issues. We easily lose impartiality, objectivity, compassion, interest, and patience. Interventional treatments are refused on “psychological” grounds. However, we have a “duty of care” and if we will not deliver it, then we should find others who will (perhaps comparable to the duty of a physician-conscientious objector to abortion to nevertheless find other caregivers for the patient). Overcoming the negativity can be very difficult when addressing the pain problems of the addicted patients who, for example, usually do not have interesting problems, are often not “nice” patients to treat, may be difficult to trust, and often waste clinical time and appointments, among other issues.
The principle of double effect
In the past, doctors have extensively debated the ethics of a principle of “double effect” of opiate use in palliative care, although the evidence that this is a problem is almost nonexistent.4 (For further discussion of “double effect” see Chapter 15). In the UK it does not seem to be considered as a significant concern. However, the doctrine of “double effect” is broader, explaining the permissibility of an action that may have some benefit but might also cause harm as a side effect. A judgment has to be made between the potential benefits and the harms. Therefore, perhaps we should redefine the use of the term and apply it to the use of opioids (and other drugs) in relieving pain in the potentially dependent patient.
Opiate prescribing in the UK
As in the US, the UK has seen a substantial increase in the prescribing of opiates for non-malignant pain. There are perhaps two major causes. First, since the early 1980s, doctors have become confident in the management of the use of opiates in malignancy and this experience has been translated to non-malignant pain. Second, with the exception of gabapentinoids, there have been no significant pharmacological advances in
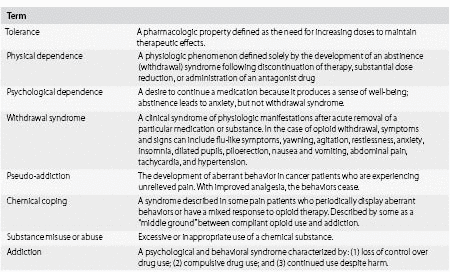
Table 25.1. Often misunderstood or misused terms in opioid dependency
pain treatment except in modes of drug delivery. The desire for simple techniques for relieving pain has led doctors, particularly pain clinicians, to see opioids as a useful and valuable option and so there has been a drift to expand their use.
In the author’s own experience, in general, prescribing habits by pain specialists have had an “educational role” and are taken up by general practitioners, albeit a year or two later. However, in general, training in the management of chronic pain is still woefully inadequate.5–7 Furthermore, few doctors, including pain clinicians, develop a comprehensive practice in the area of chronic pain in the opioid-dependent patient, because they often find the legal, ethical, and practical problems overwhelming.
Opioid dependency – a misunderstood problem
Despite the increasing recognition of chronic pain and opioid use, there is still much misunderstanding in the minds of doctors and nurses over the terminology associated with opioid dependency. Doctors still often describe patients as being addicted to their analgesics when in reality they may have some degree of dependency, but are not engaged in patterns of behavior associated with addiction (Table 25.1). Conversely, people with dependency problems may develop acute or chronic pain, acute flare-ups of chronic pain, or pain associated with malignancy, AIDS or other life-limiting diseases. Furthermore, such patients may be taking their drugs for a variety of reasons (euphoria, escapism, relief of withdrawal symptoms, medicinal purposes, or a combination). The need for training in this area has been recognized and this is incorporated into the International Association for the Study of Pain (IASP) Curriculum.8 The reality is that there are large numbers of clinicians that are highly skilled in interventional pain practice, but the same is not true for treating pain in patients with dependency.
Key differences between the UK and the US
The organization of the Health Service is a major difference between the UK and the US. All patients have a general practitioner who is the key both to ongoing prescribing and to the access to secondary care. There is a very limited role for the hospital emergency department to act as a primary health clinic and the access to a supply of opioids at this point is minimal. In hospital practice there is usually good, regular communication with the general practitioner. The normal practice would be to agree that there should only be one prescribing point for the patient. Initially, the pain clinic may manage prescribing until optimum dosing is achieved before returning this to the general practitioner. Some pain services have also developed strong links with the local addiction services to manage the addict with pain problems by running joint clinics.
Hence, in the UK, there is very little ability to go from doctor to doctor to obtain more and more prescription drugs. In practice, patients occasionally “lose” their drugs or use an excess, although they quickly learn that their requests for replacement are rarely accepted. The ability for the well off and well connected to access such drugs from private practitioners is limited. Close oversight by regulators identifies aberrant and/or high cost prescribing of opioids prescribed in primary care in locality. Prescribing opiates for registered addicts is managed through the addiction services, in general. Therefore, the access to opiates is reasonably well controlled and GPs take part in the long-term management of patients using opiates for pain, often sharing care with the pain clinics and palliative care services.
Diversion of prescribed opioids does not appear to be a great problem in the UK. In the past, problems of diversion were well recognized with short-acting opioids such as Dipipanone (Diconal), Dextromoride (Palfium) and Pethidine (Meperidine). This was resolved by either the agreed local banning of the drugs, or by agreed tight restriction in prescribing. Furthermore, it is well recognized in primary care now through education that these drugs have no use for managing chronic pain. It is notable that, in the UK, the use of diamorphine (heroin) has never been discontinued, unlike most other countries. Its use is principally within hospital practice and in palliative care. There has neither been any evidence of a significant problem with diversion nor any contribution to the widespread problems of recreational heroin use. Some addicts have been prescribed pharmaceutical grade heroin regularly to manage their addiction and there is also open debate about the possibilities of this approach to reduce their health problems. For the addict then there would be little incentive to exchange a quality product for other street drugs.
In contrast, the mild opioid, Dextropropoxyphene, combined with Paracetamol is widely used and well tolerated by many patients. It has been withdrawn recently because of concerns over its potential lethal effect when taken in deliberate overdose. The withdrawal of the drug led to many patients suffering increased pain when they were unable to find a suitable alternative. The regulatory authorities however, did not appear to engage in any debate on the ethics of this with pain clinicians. There are many other aspects of modern life that are useful and safe, but dangerous in the hands of the irresponsible. The drug alcohol and the automobile are two good examples.
Professional guidelines
The clinician trying to treat the problem patient with opioid dependency will find little evidence from clinical trials to guide pain management. What information there is has been extensively reviewed but the advice and guidance available are based on opinion and consensus.9, 10 We are left in a situation where we are often faced with complex patients with complex problems and with limited resources and abilities to manage them. Trying to do the best for these patients is not determined by long-established medical and scientific principles. The American and British Pain Societies have however, produced guidelines giving practical advice.11, 12
The British Guidelines also give examples of specific patient problems and how to deal with them. However, most patients present with a number of interconnected issues that are not easily resolvable, as in our case examples. The objective of achieving good pain control, good coping skills, and compliant, limited drug use is usually unattainable. Therefore, compromise and pragmatism are often needed to contain unsolvable problems. If this is supported by the explicit use of ethical principles, it may be possible to find the optimum way forward.
In the UK, Clinical Ethics Committees are still emerging and evolving. They have commonly provided an advisory service to the clinician to help with decision-making but in general, do not hand down formal judgments. Unfortunately, most public debate of ethical issues seems to revolve around exotic problems at the extremes of life rather than the everyday problems of clinical practice. Occasionally, clinicians refer complex cases to the courts for a decision, thereby obtaining the protection of the law, but in reality, handing over medical problems to nonclinicians.
Case resolution – UK perspective
Case 1
After getting to know Alesha, we discussed the use of strong opioids, recognizing the risks. She opted for transdermal fentanyl and settled at a stable dose. Unfortunately she developed skin problems and had to discontinue the drug. She used oral ketamine for a short period but disliked its effect on her. She moved to slow release morphine twice a day, having originally been reluctant to have access to a quantity of tablets. In this way her autonomy was respected in her participation in the management of her care.
Her general practitioner prescribed the medication under the pain clinic’s instruction, and was the only source of supply thereby reducing harm. Having originally been seen at 4-weekly periods, she is now seen in the pain clinic every 3 months. She is happy and confident with her current progress and pain control, as is her social worker and she has had fairness in her treatment. This approach has also helped improve her relationship with her general practitioner.
Case 2
Ian had a chaotic lifestyle. The opioid helped his back pain as did his alcohol. There was no other treatment that would be of help to his back in these circumstances as he was not suitable for vertebroplasty. On the ward he was accurate in his description of his opioid usage (confirmed by his general practitioner). He was also clearly suffering severe alcohol withdrawal symptoms.
We restarted his regular morphine dose (to treat pain and prevent opioid withdrawal), and quickly controlled his alcohol withdrawal symptoms (with chlordiazepoxide and other supportive measures). His symptoms and his abusive behavior settled. His general physical condition improved and he was discharged home. He was lost to follow-up in pri–mary care.
Normally, opiate prescription for primary opioid addiction would be in the hands of addiction services and not the general practitioner. Here, the opioid was used for pain. It can be considered that controlling some of his pain with morphine was better for him than his using alcohol for the same purpose therefore being beneficent. Two risks of harm are possible: diversion to pay for alcohol, and overdose. His right to use a medicine that helped his pain was negotiated and managed by his general practitioner. Restarting his morphine on the ward was beneficial to him (and to those around) and it was helpful to have recognized and treated his dependency. The duty of care was met. The general practitioner will continue the long-term care as best he can.
Case 3
Perhaps the most important ethical principle in managing Peter is fairness in management, however limited, within the medical services. He was not a friendly individual. He had been offered and had tried other treatments thereby fulfilling his right to appropriate management of his problem. Dose escalation was not an option, as it was very unlikely to provide any improvement in pain control. His threat to obtain street opioids was unlikely to be carried through as his mobility and finances were limited.
In the UK, admitting cannabis use to a medical practitioner is not uncommon and, in some communities, its use is so widespread, it would be reasonable to include it in a review of a patient’s pharmacological pain management. Its use here is probably recreational/euphoric as much as therapeutic. This then can be seen as beneficial for him in helping him cope. However, prescribing a substitute would likely be ineffective through his need to get some form of “high.” The likelihood of harm from this is minimal (nonmaleficence). Therefore, accepting its use and the overall safety of the drug in comparison to most others in routine use for pain, is the current management approach. He will continue to be seen regularly to support the general practitioner in his management (duty of care).
Key points
• Ethical problems presented by opioid-dependent patients who are suffering pain are challenging, but can be guided by simple principles of ethical medical practice.
• A patient’s dependency problem is not a justification for denying appropriate pain management. Clinicians have a “duty of care” to try to achieve pain control.
• Appropriate pain control benefits both the patient and those surrounding them. Containment of aberrant behaviors may be the best that can be achieved; however, containment is better than deterioration
• A major problem with pain management in the patient with opioid dependency is lack of physician knowledge about appropriate prescribing; education of physicians is key to developing reasonable prescribing practices.
• A principle like that of “double effect” might be useful in defining appropriate physician behavior in relieving pain in the potentially dependent patient.
Notes
a These are real examples from a single UK clinic. In this chapter, Dr. Notcutt discusses management of the cases from a UK perspective incorporating basic clinical ethics. In the following chapter, the same cases will be discussed by Dr. Ballantyne from a US perspective. The UK perspective presents what actually happened, while the US perspective presents how the cases may be handled differently by a physician in the US, understanding that opinion and practice vary considerably even within a single practice, and certainly across any single nation.
References
1 Bolam v. Friern Hospital Management Committee [1957] 1 WLR 583. The Bolam test states that if a doctor reaches the standard of a responsible body of medical opinion, he is not negligent.
2 Bolitho v. City and Hackney Heath Authority [1998] 9 MLR 26 (HL). In this judgment, it was determined that a judge must be satisfied that the body of expert opinion relied upon must have some demonstrable logical basis, and is not accepted solely because it comes from an expert body.
3 Hurwitz, B. (2004). How does evidence based guidance influence determinations of medical negligence? BMJ, 329, 1024–8.
4 Fohr, S.A. (1998). The double effect of pain medication. J Palliat Med, 1, 315–28.
5* The Pain Education Special Interest Group of the British Pain Society. (2009). Survey of undergraduate pain curricula for healthcare professionals in the United Kingdom. The British Pain Society, London UK.
6* Annual Report of the Chief Medical Officer on the State of Public Health 2008. Department of Health Publications (2009) pp. 33–39 [www.dh.gov.uk].
7 Notcutt, W. and Gibbs, G. (2010). Inadequate pain management: myth, stigma and professional fear. Postgrad Med J (accepted for publication).
8 Charlton, J.E. (ed). (2005). Core Curriculum for Professional Education in Pain, Seattle: WA, IASP Press.
9 AAPM Clinical Guidelines for the Use of Chronic Opioid Therapy in Chronic Noncancer Pain. APS Evidence Review American Pain Society. opioid/pub/pdf/org.ampainsoc.WWW_final_evidence_pdf.report.
10 Ballantyne, J. and LaForge, S. (2007). Opioid dependence and addiction during opioid treatment of chronic pain. Pain, 129, 235–55.
11 Clinical Guidelines for the Use of Chronic Opioid Therapy in Chronic Noncancer Pain. (2009). American Pain Society – American Academy of Pain Medicine Opioids Guidelines. J Pain, 10(2),113–30.
12 Pain and substance misuse: improving the patient experience. (2006). London UK: British Pain Society.
Further reading
AAPM Council on Ethics. (2005). Ethics charter from American Academy of Pain Medicine. Pain Medicine, 6(3), 203–12.
American Pain Society. (2009). Clinical guidelines for the use of chronic opioid therapy in chronic noncancer pain. American Academy of Pain Medicine Opioids Guidelines. J Pain, 10(2), 113–30.
American Pain Society. Evidence Review: APS-AAPM Clinical Guidelines for the Use of Chronic Opioid Therapy in Chronic Noncancer Pain. www.ampainsoc.org/pub/pdf/opioid_final_evidence_report.pdf.
Bannister, J. (2005). Running a pain and dependency clinic. In Managing Pain and Addiction – Opening Pandora’s Box. University of Dundee. Conference communication.
British Pain Society. (2006). Improving the Patient Experience: Pain and Substance Misuse. London, UK.
Fishbain, D. (2003). Chronic opioid treatment, addiction and pseudo-addiction in patients with chronic pain. Psychiatric Times Newsletter, 20, 2.
Littlejohn, C., Baldacchino, A., and Bannister, J. (2004). Chronic non-cancer pain and opioid dependence. J Roy Soc Med, 97, 62–5.
Portenoy, R.K. (2006). Opioid therapy for chronic non-malignant pain: clinicians’ perspective. J Law Med Ethics, 24(4), 296–309.