39–1. Which of the following is a significant risk for perioperative pulmonary complications?
a. 25 pack-year smoking history
b. Asthma well controlled with medication
c. Community-acquired pneumonia 6 months ago
d. All are significant risks
39–2. Preoperative chest radiography may be indicated in which of the following clinical settings?
a. New-onset dyspnea
b. 10 pack-year history of smoking
c. American Society of Anesthesiologist (ASA) status 2
d. All preoperative patients
39–3. Which of the following is true of methods to prevent postoperative pulmonary complications?
a. A smoking-cessation duration of less than 6 months prior to surgery does not significantly alter complication rates.
b. Routine use of nasogastric tube suctioning postoperatively is associated with higher complication rates compared with selective use.
c. Postoperative intermittent positive-pressure breathing (IPPB) lowers complication rates to a greater degree than incentive spirometry.
d. Early ambulation is as effective for pulmonary embolism prevention as intermittent pneumatic compression stockings in those with risk factors for thromboembolic disease.
39–4. Which of the following preventive measures related to cardiac disease lowers perioperative morbidity and mortality rates?
a. Maintaining hemoglobin level above 10 g/dL in those with cardiac disease
b. Intraoperative use of monopolar energy rather than bipolar energy in those with pacemaker devices
c. Initiation of perioperative beta-blocker use for all with an elevated Revised Cardiac Risk Index (RCRI)
d. Preoperative antibiotic endocarditis prophylaxis for those with valvular heart disease undergoing genitourinary procedures
39–5. In women with classic iron deficiency anemia, which of the following values is elevated?
a. Serum iron level
b. Serum ferritin level
c. Mean corpuscular volume
d. Total iron binding capacity
39–6. Which of the following regimens will most effectively correct the anemia shown here?
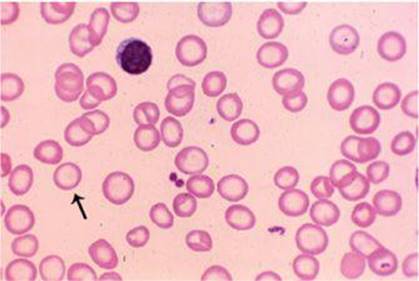
Reproduced, with permission, from Lichtman MA, Shafer JA, Felgar RE, et al (eds): Lichtman’s Atlas of Hematology. New York, McGraw-Hill, 2007, Figure I.C. 80.
a. Folate, 1 mg orally daily
b. Cyanocobalamin, 1000 g IM monthly
c. Ferrous sulfate, 325 mg orally two times daily
d. Ferrous fumarate, 200 mg orally three times daily
39–7. In patients with type 1 diabetes mellitus, postoperative insulin administration using a sliding scale should strive to maintain blood sugars below what level?
a. 100 mg/dL
b. 200 mg/dL
c. 250 mg/dL
d. 300 mg/dL
39–8. For those with adrenal insufficiency, which of the following is true regarding perioperative corticosteroid replacement?
a. All patients chronically taking oral corticosteroids require replacement prior to all surgical procedures.
b. All patients chronically taking oral corticosteroids require replacement only prior to major surgical procedures.
c. Only those chronically taking 5 mg or more of prednisone daily require supplementation for all minor and major surgical procedures.
d. None of the above
39–9. During informed consent, documentation of patient refusal for a specific procedure should include all EXCEPT which of the following?
a. Documentation of the reason for the patient’s refusal
b. Documentation that the patient refused the recommended intervention
c. Documentation that the intervention and its value were explained to the patient
d. Documentation that the patient will be discharged from the provider’s care following the refusal
39–10. Preoperative antibiotic prophylaxis is recommended for which of the following procedures?
a. Total laparoscopic hysterectomy
b. Ovarian cystectomy via laparotomy
c. Hysteroscopic myomectomy of a type 0 lesion
d. Laparoscopic tubal application of Filshie clips
39–11. Prior to total abdominal hysterectomy, all EXCEPT which of the following are suitable preoperative intravenous antibiotic prophylaxis regimens?
a. Cefoxitin 2 g
b. Clindamycin 600 mg
c. Clindamycin 600 mg plus ciprofloxacin 400 mg
d. Metronidazole 500 mg plus gentamicin 1.5 mg/kg
39–12. Risk factors for venous thromboembolism (VTE) include all EXCEPT which of the following?
a. Pregnancy
b. Tamoxifen therapy
c. Copper intrauterine device
d. Ovarian hyperstimulation syndrome
39–13. Of the thrombophilias, which is the most thrombogenic?
a. Protein C deficiency
b. Antithrombin deficiency
c. Prothrombin G20210A mutation
d. Activated protein C resistance (factor V Leiden mutation)
39–14. Of the thrombophilias, which is the most prevalent?
a. Protein C deficiency
b. Antithrombin deficiency
c. Prothrombin G20210A mutation
d. Activated protein C resistance (factor V Leiden mutation)
39–15. In evaluation of patients for thromboembolism prophylaxis, all EXCEPT which of the following are major considerations?
a. Minor versus major surgery planned
b. Coexistent venous thromboembolism risks
c. General versus regional anesthesia planned
d. Laparoscopic versus open surgical approach planned
39–16. According to the American College of Chest Physicians 2008 guidelines, for patients with no venous thromboembolism (VTE) risks who are undergoing major gynecologic surgery, all EXCEPT which of the following are suitable VTE prophylaxis?
a. Low-molecular-weight heparin
b. Low-dose unfractionated heparin
c. Graduated compression stockings
d. Intermittent pneumatic compression
39–17. Findings suggestive of a prerenal source for postoperative oliguria include all EXCEPT which of the following?
a. Tachycardia
b. Orthostatic hypotension
c. Urine sodium of 15 mEq/L
d. Fractional excretion of sodium greater than 3 percent
39–18. Eight hours following an uncomplicated total abdominal hysterectomy for large uterine leiomyomas, you notice that your patient has a temperature of 37.8°C during your postoperative check. She is asymptomatic, her pulse is 88, respiratory rate is 12, and her blood pressure is 132/78. Her lungs are clear during auscultation, her urine appears clear and copious, and her wound shows no bleeding or erythema. Which of the following is an appropriate response?
a. Order a chest radiograph
b. Initiate broad-spectrum antibiotics
c. Order chest computed tomography angiography
d. Encourage deep breathing and continue observation
39–19. All of the following organisms may commonly be the primary pathogen for hospital-acquired pneumonia, EXCEPT for which gram-negative coccobacillus shown here?

Reproduced, with permission, from Levinson W: Gram-negative rods related to the respiratory tract. In Review of Medical Microbiology and Immunology, 11th ed. New York, McGraw-Hill, 2010, Figure 19-1.
a. Escherichia coli
b. Klebsiella pneumoniae
c. Pseudomonas aeruginosa
d. Haemophilus influenzae
39–20. Following total abdominal hysterectomy for uterine leiomyomas, your patient complains of dyspnea on postoperative day 1. Her respiratory rate is 33, oxygen saturation is 88 percent on room air, pulse rate is 98, and her temperature is 38.3°C. She has no prior or family history of thromboembolism or thrombophilia. Her chest radiograph is shown below. Which of the following is the most appropriate next step?

a. D-Dimer measurement
b. Chest computed tomographic (CT) angiography
c. Initiate antibiotics with gram-negative coverage
d. Encourage deep breathing and continue observation
39–21. Below is the computed tomographic (CT) angiogram from the patient in Question 39–20. You initiate pulmonary support and anticoagulation therapy. How long postoperatively should her anticoagulation therapy be continued?

Reproduced, with permission, from Cunningham FG, Leveno KL, Bloom SL, et al (eds): Thromboembolic disorders. In Williams Obstetrics, 23rd ed. New York, McGraw-Hill, 2010, Figure 47-5.
a. 6 weeks
b. 3 months
c. 6 months
d. Indefinitely
39–22. Postoperatively, if deep-vein thrombosis is suspected, which of the following diagnostic tests (shown here) is initially preferred?
a. Venography
b. Duplex sonography
c. Magnetic resonance imaging
d. Impedance plethysmography

Reproduced, with permission, from Moschos E, Twickler DM: Techniques used for imaging in gynecology. In Schorge JO, Schaffer JI, Halvorson LM, et al (eds): Williams Gynecology, 1st ed. New York, McGraw-Hill, 2008, Figure 2-21.
39–23. Routine use of which of the following is an effective strategy in the treatment of ileus?
a. Gum chewing
b. Nasogastric tube suctioning
c. Intravenous fluids and electrolyte repletion
d. All of the above
39–24. In general, which of the following is the most common type of shock encountered in gynecology?
a. Septic
b. Neurogenic
c. Hypovolemic
d. Cardiogenic
39–25. For patient with hypovolemic shock, which of the following is selected for initial intravenous resuscitation?
a. Whole blood
b. Isotonic crystalloids
c. Hydroxyethyl starch (hetastarch) colloid solution
d. None of the above
39–26. Clinical signs of superficial wound infection commonly include all EXCEPT which of the following?
a. Drainage from the wound
b. Erythema surrounding the wound
c. Petechial rash surrounding the wound
d. Superficial separation of wound edges
39–27. Initial steps of superficial wound infection treatment include all EXCEPT which of the following?
a. Antibiotic treatment
b. Evacuation of hematomas
c. Debridement of devitalized tissue
d. Wound reapproximation with delayed-absorbable suture
39–28. Six days following total abdominal hysterectomy through a midline vertical incision, your patient presents with an erythematous wound with scant purulent drainage. During examination, the wound spontaneously opens (shown here) and copious foul serosanguinous fluid spills. Her temperature is 38.2°C. Because of concerns for fascial dehiscence, she is taken to the operating room for debridement of her incision and examination of the fascia. Integrity of the fascial incision is documented. Antibiotics selected for this patient should cover which of the following pathogens?
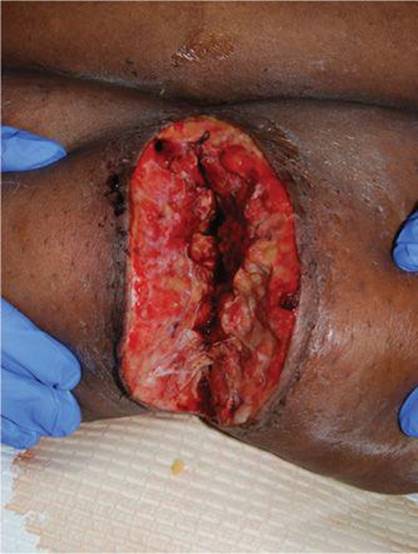
a. Solely gram-positive bacteria
b. Solely gram-negative bacteria
c. Anaerobic and gram-positive bacteria
d. Anaerobic, gram-positive, and gram-negative bacteria
39–29. The wound technology shown here offers which advantages?
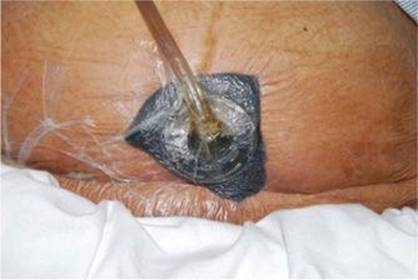
a. Removes exudates
b. Prompts wound retraction
c. Stimulates granulation tissue formation
d. All of the above
Reference
Geerts WH, Bergqvist D, Pineo GF, et al: Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Ed.). Chest 133(6 Suppl):381S, 2008.
Chapter 39 ANSWER KEY
