Alexander McMillan1, 2
(1)
Department of Genitourinary Medicine, NHS Lothian, Edinburgh Royal Infirmary, Edinburgh, Uk
(2)
University of Edinburgh, Edinburgh, Uk
Alexander McMillanFormerly, Consultant Physician, part-time Senior Lecturer
Email: a.amcmm@btinternet.com
Abstract
A 21-year-old man, James, attends a Sexual Health clinic with a 4-day history of severe pain on urination, associated with general malaise and feverishness. He does not have frequency of micturition, urgency, hesitancy, frank hematuria, or abdominal pain. He had unprotected receptive oral sex with a young woman whom he had met at a party 7 days previously; he did not have genital–genital contact with her. Before that encounter, his most recent sexual contact had been some 6 months previously with an ex-girlfriend.
A 21-year-old man, James, attends a Sexual Health clinic with a 4-day history of severe pain on urination, associated with general malaise and feverishness. He does not have frequency of micturition, urgency, hesitancy, frank hematuria, or abdominal pain. He had unprotected receptive oral sex with a young woman whom he had met at a party 7 days previously; he did not have genital–genital contact with her. Before that encounter, his most recent sexual contact had been some 6 months previously with an ex-girlfriend.
He looks well. His temperature is 37.5°C. There is no skin rash and no conjunctivitis. There is marked meatitis (Fig. 23.1 ) and a mucoid urethral discharge. Genital ulceration is not noted. Several lymph nodes in the left inguinal region are enlarged and tender. Dipstick analysis shows no proteinuria, hematuria, or glycosuria.
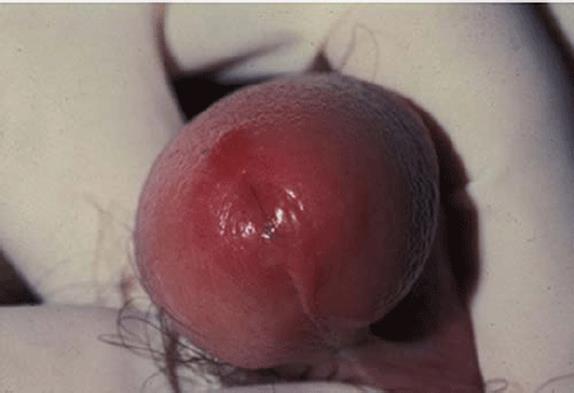
Figure 23.1.
Meatitis.
Microscopy of a Gram-stained urethral smear shows about 5 polymorphonuclear leucocytes per ×1,000 field; Gram-negative diplococci are not identified.
23.1 What Two Sexually Transmissible Infections Would You Consider as the Most Likely Cause of His Urethritis?
The severity of the dysuria with the finding of urethral meatitis and inguinal lymphadenopathy suggests the possibility of either herpes simplex virus (HSV) infection or adenovirus infection. Both primary HSV infection1 and adenovirus infection may be associated with systemic symptoms as in this case. As the pre-patent period for both infections is short – between 4 and 10 days – consideration of this does not help in the differential diagnosis. The absence of external genital ulceration does not exclude urethral HSV infection that could have been acquired through oral–genital sexual contact. (In industrialized countries, almost half of all cases of primary genital herpes in young adults are caused by HSV type 1). Adenovirus infection can cause upper respiratory disease, and sometimes conjunctivitis. Urethral infection may result from insertive oral–genital contact with an individual who is excreting virus from the upper respiratory tract. (It is known that viral shedding can occur for a prolonged period after the initial infection). Although there have been several case reports of adenovirus-associated urethritis with conjunctivitis, the absence of the latter feature in this case does not exclude the diagnosis.
The severity of the dysuria with minimal signs argues against a diagnosis of urethral gonorrhea, a conclusion supported by the absence of Gram-negative diplococci in the Gram-stained smear.
Urethral infection with the oculogenital genotypes of Chlamydia trachomatis is unlikely to be associated with such severe dysuria. In any case, C. trachomatis is found uncommonly in the oropharynx, and the risk of transmission to the urethra during fellatio is considered to be small. Although there have been outbreaks of anorectal infection with the lymphogranuloma venereum genotypes of C. trachomatisamongst men who have sex with men, urethral infection appears to be rare, and the sexual history makes this a most unlikely diagnosis in this case.
23.2 How Would You Manage This Case?
Urethral material should be obtained from the urethra for the detection of HSV and adenovirus DNA by nucleic acid amplification methods. Although Gram-negative diplococci were not identified in smear microscopy, culture or a NAAT for Neisseria gonorrhoeae should be performed. A first-voided specimen of urine should also be obtained for the detection of C. trachomatis DNA.
Adenovirus infection is self-limiting and antiviral agents are not available for use in urethral infection. As the differential diagnosis includes HSV infection, he should be given a 5-day course of aciclovir, valaciclovir, or famciclovir (see Case 16). Many physicians would also give either a single oral dose of azithromycin or a 7-day course of doxycycline.
He returns to the clinic 7 days later. His symptoms have resolved, and the urethral meatus appears normal. HSV-1 was detected in the swab taken from the urethra, but the laboratory tests for adenovirus, N. gonorrhoeae, and C. trachomatis were negative. He was counseled about genital herpes as described inCases 16 and 17.
Footnotes
1
This is an infection in an individual who has not been previously infected with either HSV type 1 or HSV type 2.