DEBRA BOYER
ALICIA CASEY
HISTORY OF PRESENT ILLNESS
The patient is a 7-month-old girl, who was well until 4 days prior to presentation. At that time, she developed a cough with fevers to 40.5°C. On the day of presentation, she developed wheezing and a rash on her trunk and face. This rash began on her chest and spread to her face. Over the preceding 4 days her cough had increased significantly. She received nebulized albuterol twice at home without relief. She had poor oral intake and urine output.
MEDICAL HISTORY
She was the full-term product of an uncomplicated vaginal delivery. She was brought to the emergency department three times for wheezing episodes. Her only medication was nebulized albuterol. At the time of presentation, the patient and her family were living in a shelter. A roommate at the shelter was recently hospitalized with a rash, fever, and pneumonia.
PHYSICAL EXAMINATION
T 40.6°C; P 168 bpm; RR 60/min; BP 102/55 mmHg; Oxygen saturation 99% in room air
Weight 50th percentile; Height 75th to 90th percentile
Initial examination revealed an alert baby, who was crying, but consolable. She appeared slightly pale. Physical examination was notable for an erythematous right tympanic membrane and bilaterally injected conjunctiva with yellow discharge. She had moderate rhinorrhea and some notable buccal thrush. Her oropharynx was mildly erythematous. Chest examination was remarkable for an elevated respiratory rate, but no retractions. She had fine expiratory wheezes bilaterally with decreased breath sounds at both bases. Her skin had a fine erythematous blanching maculopapular rash on her face and torso (Figure 4-5) and to a lesser degree on her extremities. Her palms and soles were spared. The rash appeared confluent in her perineal area and torso. The remainder of her physical examination was unremarkable.
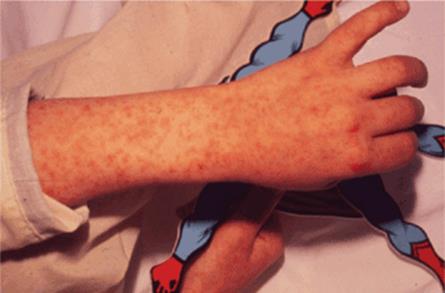
FIGURE 4-5. Example of a rash.
DIAGNOSTIC STUDIES
Laboratory analysis revealed a peripheral blood count with 10 900 white blood cells/mm3 with 41% segmented neutrophils, 50% lymphocytes, 8% monocytes, and no band forms. Her hemoglobin was 10.6 g/dL and there were 290 000 platelets/mm3. A urinalysis was normal and a chest roentgenogram revealed mild hyperinflation, right middle lobe atelectasis, and some peribronchial cuffing.
COURSE OF ILLNESS
The patient received two nebulized albuterol treatments without significant change in her respiratory status. Blood and urine cultures were sent to the laboratory and revealed no growth. Her fever resolved during the next 2 days, her rash faded, and her respiratory status began to normalize. She was discharged after a 4-day hospitalization. Examination of the rash (Figure 4-5) suggested a diagnosis that was confirmed by blood work obtained during her hospitalization.
DISCUSSION CASE 4-3
DIFFERENTIAL DIAGNOSIS
Viral infections are the most common cause of a cough in infancy, with rhinovirus, coronavirus, respiratory syncytial virus, parainfluenzae, human metapneumovirus, and influenza among the leading agents. These viruses also commonly produce lower airway disease in infants, and thus, bronchi-olitis often accompanies the cough. With bronchi-olitis, infants frequently present with decreased aeration, diffuse crackles, and wheezing appreciated on auscultation. Fever and profuse rhinorrhea are common.
Other infectious etiologies are possible and should be considered in the differential diagnosis, including C. trachomatis, pertussis, and bacterial pneumonia. Less commonly, infants will present with pulmonary tuberculosis and fungal infections. Rarely, infectious entities such as measles or parasitic infections will present with cough.
While cough can be the presenting symptom with congenital malformations and underlying lung disease, this patient’s presentation strongly suggested an infectious etiology. The features of this case that prompted additional evaluation included the rash and associated respiratory findings.
DIAGNOSIS
The rash was characteristic of measles (Figure 4-5). Antibody titers to measles were sent on admission and were negative. Repeat titers were sent prior to her discharge on hospital day 4. IgM antibodies specific for measles were found to be positive. The diagnosis is measles.
INCIDENCE AND EPIDEMIOLOGY
Measles is the infectious condition caused by the rubeola virus, an RNA virus of the family of para-myxoviridae. Measles remains endemic outside of North and South America. Prior to the introduction of the measles vaccine in 1963, 200 000-300 000 cases of measles were recorded each year in the United States. Since the measles vaccines usage, measles in the United States has dramatically decreased by 99%. By the year 2000, endemic transmission ended. Since then, there has been a median of 60 cases per year from 2001 to 2010. Unfortunately, there was a dramatic increase in the number of cases (222) and outbreaks (17) in 2011. Most recent cases of measles occurring in people born in the United States can be traced to imported exposure either from personal travel abroad or contact with individuals infected abroad. Exposures occurred most frequently in Europe or South East Asia. Of recent cases, most occurred in unvaccinated individuals. In the cases of unvaccinated children, many were ineligible for vaccination (too young or had a medical contraindication), the parents reported a religious or personal exemption or the patient was simply delayed in their vaccination schedule. Infrequently, cases of primary vaccine failure have been reported.
Measles is spread as an airborne virus, and thus persons become infected by direct contact with droplets from the respiratory secretions of infected patients. Measles is highly contagious and approximately 90% of susceptible people develop symptoms after exposure. The typical incubation period is 10 days (range 7-21 days). Generally, children are considered contagious from 3 days prior to the onset of the rash until 6 days after the onset of the rash. Mortality in the United States occurs about 1-2 per 1000 infections, and is more common in infants, children, and immunocompromised individuals. Hospitalization is frequently required and rates of hospitalization are highest among infants and children. Pneumonia is not uncommon and can be severe. Encephalitis is a rare, but still reported and devastating complication.
CLINICAL PRESENTATION
The prodromal phase begins with 3-5 days of malaise, fever, cough, coryza, and conjunctivitis. These symptoms increase over the course of the prodromal phase. Just prior to the development of the exanthem, Koplik spots are noted. These are bluish white spots on a red base and are found classically in the buccal mucosa, but may be found on the lips, palate, gingiva, conjunctival folds, and vaginal mucosa. Koplik spots are pathognomonic of measles. The exantham begins as Koplik spots begin to slough. The rash begins typically on the face and then moves in a caudal direction. The rash is initially erythematous and maculopapular, but then becomes confluent. The rash generally lasts 5-7 days. The most persistent symptom is often the cough.
With typical measles, patients are generally ill for 7-10 days. Other manifestations can include pharyngitis, otitis media, lymphadenopathy, croup, bronchiolitis, sinusitis, diarrhea, vomiting, and dehydration. Febrile seizures can occur. However, more severe complications can occur and include pneumonia, bronchiolitis obliterans, tracheitis, mastoiditis, retropharyngeal abscess, appendicitis, acute encephalitis, myocarditis, pericarditis, hemorrhagic skin eruption, and keratitis. Measles during pregnancy is associated with increased maternal morbidity, fetal demise, and congenital malformations. Subacute sclerosing panencephalitis (SSPE) is a rare delayed neurologic complication of measles infection. This complication is fatal in most cases. SSPE consists of a degenerative CNS process that is associated with a persistent intra-cellular measles infection and can present years after infection.
DIAGNOSTIC APPROACH
The diagnosis of measles is generally based on clinical presentation and having a high index of suspicion for diagnosis. Often measles goes undiagnosed due to infrequent cases and confusion with other common illnesses presenting with rash and fever. Identification of cases is essential to limit spread and prevent outbreaks. For these reasons, all suspected cases should be confirmed. All known or suspected cases of measles should be reported to the State Health Department and the Center for Disease Control (CDC).
Serologic titers. Confirmation of measles infection can be made most conveniently by detecting measles-specific immunoglobulin M (IgM) in the serum. This is the most common method of diagnosis. Depending on the sensitivity of the assay, antibodies can be detected within 1-3 days after onset of rash. Measles IgM generally peaks 10 days after rash onset and usually remains 30-60 days after rash onset. The presence of measles-specific IgM antibodies will establish the diagnosis. Analysis of acute and convalescent titers of IgG can also be used.
Clinical specimen testing/collection. Measles infection can also be confirmed by the detection of measles virus RNA by nucleic acid amplication. This testing can be done on specimens such as nasopharyngeal/oropharyngeal swabs, nasal aspirates, throat washes, or urine. Virus isolation is best performed 1-3 days after onset of rash, but can be detected up to 7 days post. Clinical specimens can also be used to determine source of infection based on genetic sequence data.
TREATMENT
In uncomplicated measles, patients will only require supportive care, including antipyretics and fluids. Antibiotics are only necessary in cases of bacterial superinfection, particularly pneumonia. Typical organisms causing a superinfected bacterial pneumonia include Streptococcus pneumoniae, Staphylococcus aureus, Haemophilus influenzae, and Streptococcus pyogenes. Vitamin A deficiency has been associated with increased mortality and treatment with this has been shown to reduce mortality and complications. Treatment with vitamin A may be recommended for certain individuals.
PREVENTION
The measles, mumps, rubella (MMR) vaccination is administered at age 12-15 months with a second dose at 4-6 years. It is recommended that infants older than 6 months be administered the vaccine if international travel is planned. This vaccine is highly effective. Exposed susceptible individuals may be treated with vaccination and passive immune globulin.
SUGGESTED READINGS
1. Regamey N, et al. Viral etiology of acute respiratory infections with cough in infancy: a community-based birth cohort study. Pediatr Infect Dis J. 2008;27(2): 100-105.
2. Wilbert HM: Measles. In: Kliegman RM, Stanton BMD, St. Geme J, Schor N, Behrman R, eds. Nelson Textbook of Pediatrics. 19th ed. Philadelphia, PA: Saunders; 2011: 1069-1075.
3. Center for Disease Control and Prevention (CDC). Measles-United States, 2011. MMWR Morb Mort Wkly Rep. 2012;61:253-257.
4. Center for Disease Control and Prevention (CDC). Measles Homepage. http://www.cdc.gov/measles/. Accessed July 15, 2012.
5. Parker Fiebelkorn A, Redd SB, Gallagher K, et al. Measles in the United States during the postelimination era. J Infect Dis. 2010;202:1520-1528.
6. Watson JC, Hadler SC, Dykewicz CA, Reef S, Phillips L. Measles, mumps, and rubella-vaccine use and strategies for elimination of measles, rubella, and congenital rubella syndrome and control of mumps: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recommendations & Reports. 1998;47(RR-8):1-57.