‘You largely constructed your depression. It wasn’t given to you. Therefore, you can deconstruct it.’
Albert Ellis, American psychologist and psychotherapist
At any given time, conservative estimates state that between 15% and 20% of the adult population are suffering from significant depressive symptoms. Because depression has become so commonplace we can easily underestimate the misery it causes. The real tragedy is that so much of this distress is unnecessary. CBT offers a tried and tested model of depression and treatment strategies that have good rates of success when diligently applied.
You may remember from Chapter 1 that Beck pioneered CBT as a treatment for depression back in the sixties. His original formulation of depression and the techniques he devised for tackling it have scarcely been modified since then, although recently combining CBT with practices borrowed from the Eastern meditation practice known as mindfulness are producing promising results, especially when it comes to preventing relapse.
Are you depressed?
We all feel down from time to time, but to establish whether you might be suffering from clinical depression have a look at the following checklist:
□ Do you feel consistently low most days?
□ Do you find it hard to motivate yourself and take pleasure in things?
□ Have you lost or gained significant amounts of weight recently? (People who are depressed either lose their appetite or tend to comfort eat.)
□ Are you sleeping much more or less than usual?
□ Do you feel restless, jittery and unable to settle much of the time or find yourself feeling unusually sluggish and listless?
□ Do you feel tired and drained most days?
□ Do you feel especially worthless or guilty?
□ Are you finding it hard to concentrate and remember things at the moment?
□ Do you have recurrent thoughts about dying (even if you have no intention of acting on them)?
If you answered yes to five or more of these questions and your symptoms have persisted for at least two weeks then the chances are you may be suffering from a major depressive episode.
Depression is a serious illness. It currently accounts for 75% of all admissions to psychiatric wards and severe depression can even be accompanied by psychotic episodes when people lose touch with reality and may experience delusions or hallucinations. While obviously only a tiny minority of cases become anywhere near this extreme, these statistics do emphasise that depression should not simply be ignored.
The longer depression is left untreated the harder it becomes to deal with. If you think you are suffering from clinical depression don’t suffer in silence. Hopefully, the techniques described in this chapter will be of help to you, but do talk to your GP if you feel your symptoms are not shifting; your GP will be able to refer you to a suitable therapist.
It is worth noting that there are various forms of depression. People who suffer from bipolar depression typically find that they alternate between crashing lows and periods when they are filled with manic energy. At such times people tend to feel great but often find themselves acting in impulsive or irresponsible ways – wild spending sprees and indiscrete sexual behaviour are not uncommon during manic phases. However (perhaps unfairly) not everyone who suffers from a bipolar disorder experiences the manic highs but may still require specialist treatment.
If you think you are depressed it is worth talking to your doctor who can advise you regarding appropriate investigations and treatment options.
A word about drugs
You do not have to choose between taking prescribed antidepressants and using cognitive behavioural techniques. Trials by the National Institute of Clinical Excellence established that for most people a combination of CBT and antidepressants is often the most effective treatment. In practice some people find that with antidepressants taking the edge off their organic depressive symptoms they can actually make better use of CBT techniques.
Obviously the decision to take any kind of medication is a personal call, but some individuals put themselves under enormous unnecessary pressure in relation to this issue. Remember you can always try medication and if, on balance, you find it helps you then all well and good. However, if the side effects start outweighing the benefits you can always go back to your GP to consider alternative ways forward. If you have doubts about the merits of medication, talk them through with your doctor. This commits you to nothing but will equip you to make a more informed choice.

Duncan was the youngest in his family. His birth was not planned and his parents were both a bit shell-shocked when his mother fell pregnant at the age of 46. They weren’t prepared to have to revisit nappies and sleepless nights, especially since his eldest brother had just set off for university and they were looking forward to having time to pursue their own interests.
Unfortunately their resentment had communicated itself to Duncan. Deep down he felt unwanted and an inconvenience to his family. (‘There was always this slight sense of three’s a crowd…’) Nevertheless, Duncan was a bright and popular child and did well at school. His childhood was generally unremarkable and, despite sometimes appearing rather driven, he appeared a happy, well-adjusted boy.
Duncan met Jennifer at college and they married shortly after they graduated. He got a sought-after post in a prestigious marketing company. Everything seemed to be going well for the young couple, and one day when he returned from work Jennifer announced that she was expecting a baby.
Both parents were delighted, but shortly after the birth of their daughter, Molly, Duncan noticed that his mood was changing. He felt fed up and became uncharacteristically snappy. Jennifer was constantly busy with Molly and, although he loved his daughter, Duncan found himself feeling increasingly resentful of how little time they had together. ‘I just feel a bit shut out,’ he complained. Friends told him this was entirely normal in the early months and Duncan dismissed his low mood as a function of disrupted sleep and adjusting to the upheaval of a new baby.
However, as the weeks went by, things got worse. Duncan became more and more withdrawn. He found it hard to concentrate at work and at weekends he could hardly drag himself out of bed – which inevitably became a real issue for Jennifer who understandably felt she wanted some help with Molly having looked after her all week.
The family struggled on, but over the next few months a downturn in the economy started to make Duncan’s position at work look increasingly vulnerable. During a recent performance review his boss had expressed concern about their declining sales figures and Duncan became obsessed with fears about being made redundant, even though there were no indications that this was likely. ‘I know I am not coping with anything any more,’ he told me. ‘It can only be a matter of time before they realise what a liability I am and chuck me out. Then what’s going to happen to us? It doesn’t bear thinking about. Maybe it would be better for everyone if I just didn’t exist…’ Looking haggard and tearful as he said this, all the evidence pointed to the fact that Duncan was now in the grip of a major depressive episode.
Beck’s model of depression
Beck proposed that some people are often vulnerable to depression because of negative assumptions laid down in childhood. Under normal circumstances, he suggested, these beliefs may lie dormant but a critical incident is all it takes to activate them and unleash a stream of associated negative thoughts. Repeated exposure to these thoughts, Beck argued, in due course produces the organic, physical symptoms of a depressive disorder.
In Duncan’s case, his parents’ reaction to having an unplanned child had contributed to assumptions and core beliefs about being unwanted and unvalued. These niggling misgivings had not troubled him unduly during his upbringing, offset as they were by many other positive experiences. He had felt secure in his peer group and felt that his good grades at school gave him tangible proof of his worth, especially since his marks had also earned him the approval of his parents. When Duncan met Jennifer, the intimacy between them gave him a real sense of belonging that largely buried the insecurities of his childhood and his success at work continued to build his self-esteem.
Worked example of Beck’s model of depression
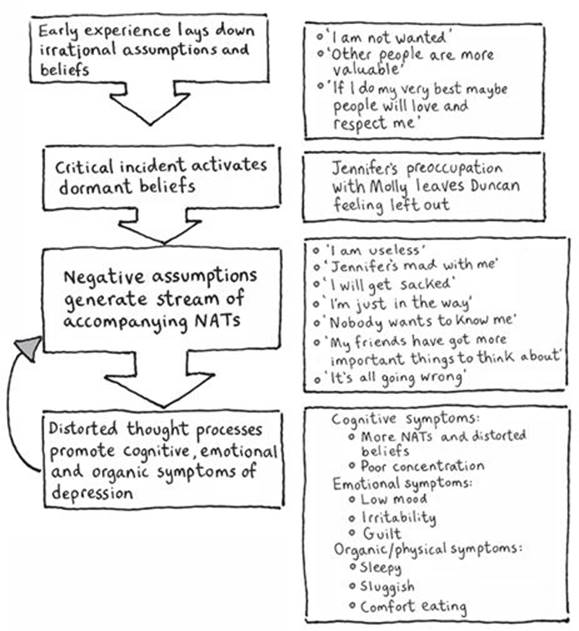
For Duncan the birth of Molly proved the critical incident that activated his childhood assumptions. Jennifer’s preoccupation with the baby triggered Duncan’s old fears of exclusion. He felt that now she had Molly, Jennifer no longer wanted or needed him. Suddenly all his negative core beliefs were up and running, producing a steady stream of unhelpful NATs that were soon dragging Duncan into a spiral of depression.
As the depression took hold, Duncan’s unhelpful core beliefs started to become self-fulfilling prophecies: his irritability and passivity at home did start to distance him from his wife while concentration difficulties and low levels of motivation laid him open to criticism at work. Since his self-esteem was so closely tied into his perceived success, the loss of his status as a rising star within the company hit him hard and made him even more susceptible to the impact of his buried core beliefs. His fears that he would ultimately be rejected professionally, as well as personally, flowed naturally from his underlying convictions: ‘I am not really wanted’ and ‘Other people are more valuable than me’.
How depressed people think
We normally think of depression as synonymous with low mood but, having read this book it will come as no surprise to learn that depression is a condition that affects how we think and behave. The poet Sylvia Plath described depression as like looking at the world through a bell jar – an image that emphasises just how distorted the thinking of a depressed person can become.
Beck noted that the thoughts of depressed people tend to reflect the following themes:
1. Critical thoughts about the self
· ‘I’m stupid.’
· ‘I’ve stuffed up again.’
· ‘No one could care about me.’
· ‘I am bad through and through.’
2. A bleak, negative view of other people and the world in general
· ‘People always let you down.’
· ‘The world is a vicious place.’
· ‘Everyone’s out for themselves.’
3. A pessimistic outlook on the future
· ‘Nothing good lasts for long.’
· ‘There’s no point trying – I will only fail.’
Maintaining factors in depression
In order to maintain these depressive assumptions, depressed people tend to use a broad repertoire of characteristic cognitive distortions including polarised thinking, filtering, personalisation and generalisation (see Chapter 3 for details).
When explaining negative events depressed people tend to hold themselves responsible – even when they are not necessarily to blame. Any mistakes they do make are magnified and taken as examples of engrained character flaws rather than a function of particular circumstances. Needless to say they see little hope that the situation will improve.
As in Duncan’s case the behaviour of depressed people only tends to reinforce the cycle of negative thinking. Because depressed people tend to become withdrawn and lethargic, they often make themselves feel worse. By behaving in this way they no longer provide themselves with experiences and opportunities that might challenge their sense of helplessness and worthlessness.
Moreover their passivity provides ample opportunity for depressed people to reflect on their shortcomings and reinforce their pessimistic thinking style. Compulsive rumination – endlessly going over the same problem-saturated scenarios – is a key characteristic of such individuals.
Taking things easy when you feel this fragile seems at face value like a sensible thing to do, but as they withdraw from everyday routines depressed people unwittingly confirm how badly they are coping with life. As a brilliant student of CBT, you will already have recognised that this is actually a classic safety behaviour, and like most safety behaviours it spells trouble.
Cognitive strategies for tackling depression
Cognitive behavioural treatments for depression usually involve a multi-pronged attack on the various maintaining factors we have just described. In the later stages of treatment, you may also find it helpful to target the core beliefs and assumptions that may have made you vulnerable to depression in the first place.
There are four main cognitive techniques for addressing depressed thinking styles:
1. decentring yourself from your depressive thoughts
2. distraction techniques to halt unhelpful rumination
3. challenging cognitive distortions using thought records
4. activating problem-solving skills to counteract feelings of helplessness.
1 Decentring yourself from your depressive thoughts
It all sounds a bit Californian, doesn’t it? What decentring actually involves is learning to step back from your depressive thoughts and observe them rather than being so immersed that you can no longer separate yourself from them.
When you are closely identified with your depressive thoughts it is almost impossible to do anything about them. When you become conscious of your depressive thoughts and feelings for what they are, i.e. just patterns of thoughts and feelings intruding into your awareness, you automatically weaken their power.
Decentring is the essence of the ‘mindfulness’ approach. Rather than trying to grapple with your thoughts, the mindfulness tradition encourages you simply to observe the flow of your consciousness while adopting an accepting, non-judgemental stance. Instead of trying to control your depressive thoughts directly you notice them, label them and allow them to pass through your mind unobstructed. This is in stark contrast with the nature of depressive rumination which usually involves mentally grabbing on to a misery-inducing scenario and making it play in your head over and over again.

An exercise conducted in the first session of many mindfulness groups involves nothing more complicated than eating a piece of fruit while concentrating fully on the experience and how it affects you. The rationale is that we spend much of our lives in a state of divided attention. A bit like a computer with several programs up and running at the same time we are quite capable of automatically running depressive processing subroutines alongside whatever else we are doing.
By learning to live fully ‘in the moment’ and gently bringing awareness back to bear on incoming sensory information (the feel of the peach in your hand, the levels of muscular tension in your body, the feeling of the warm evening breeze on your skin) the goal is to channel your awareness into a single integrated channel that diverts energy away from fruitless rumination – no pun intended.
This may strike you as deceptively easy but just try it! Mindfulness belongs to a meditative tradition long established in the east, and like all meditation practices it is a discipline that requires considerable practice to perfect. My advice is that if this approach appeals to you, then follow the link http://mbct.co.uk/the-mbct-programme and contact a local group where you can practise with the support of others and quite possibly the guidance of a suitable psychologist.
2 Distraction techniques
These involve using more active strategies to interrupt the flow of negative thinking. You can use the same kinds of sensory awareness techniques described above to anchor yourself in your surroundings. Describing in detail what you can see around you, the sounds you can hear and even tactile sensations can shift your focus away from your thoughts. Some people find that pinging an elastic band worn on the wrist whenever a depressive thought enters their head can also provide a brief, alternative, sensate focus as well as training them to become more aware of bad cognitive habits.
Alternatively you can try setting yourself a distracting mental task. Count back from a hundred in threes or try setting anagrams in your head. Tongue twisters can also provide a handy and demanding activity that will monopolise your concentration and temporarily stop depressive rumination in its tracks.
3 Challenging cognitive distortions
This involves using the skills described in Chapter 4 to counter the content of your negative thoughts and beliefs. Below is a sample thought record from Tracy, a retired nurse suffering from depression, illustrating how these techniques can be used to work towards more balanced thoughts to use as an antidote to depressive NATs.
|
Trigger |
Watching people go to work from the window |
|
Emotions |
Feel bleak 80% |
|
Resigned 60% |
|
|
Hollow feeling in pit of stomach 50% |
|
|
NATs |
‘I am no use to anyone’ |
|
‘I am a drain and a burden’ (85%) |
|
|
‘I’m all washed up’ |
Evidence supporting negative thought:
· I am not working any more.
· My children are all grown up and don’t need me.
· My hospital appointments for my rheumatism take up time and money that would be better spent on someone younger.
Evidence challenging negative thought:
· My friends seem to enjoy my company.
· Without me as bridge partner, Margaret wouldn’t leave the house day in day out.
· My value doesn’t depend on what I do but who I am.
· My children may not need me physically, but Sarah still uses me as a shoulder to cry on when the twins are getting too much for her.
· I am an active and involved grandmother.
· When I was a nurse I believed that the good thing about the NHS was that it was available to everyone – there’s no reason that shouldn’t include me.
Alternative thought/more balanced position:
‘Just because I am not working doesn’t mean my life has no value or that I am not making a valid contribution to other people’ (85%).
4 Problem-solving approaches
Feeling helpless and disenfranchised is one of the characteristic feelings of depressed people. They can feel that they have no resources to tackle problems in their own lives or those of anyone else. Consciously using problem-solving strategies can make even depressed individuals feel more empowered. For example, if your negative thoughts are telling you that the world is a bleak uncaring place, try brainstorming things you personally could do to make a difference – perhaps volunteering for a charity or even just writing a letter to a friend. There are often constructive ways forward even with personal situations that feel hopeless, despite what your depression would tell you. Try to identify three things you could do that would improve your situation, however slightly. If you are struggling to do this, why not enlist the help of a practically minded friend or relative who could help you come up with some ideas?
Behavioural strategies for tackling depression
Behavioural approaches are indispensable when tackling depression. One study found that people who used the behavioural techniques described below reported higher rates of symptom relief than those who exclusively used a cognitive approach. Obviously this is a bit of a false distinction since, as you have learned, behavioural interventions do directly impact on our thoughts and feelings. However, the point is that when it comes to sorting out depression, what you do is just as important, if not more important, than mental strategies alone. Behavioural techniques include:
1. activity scheduling
2. behavioural experiments to challenge depressive assumptions
3. exercise.
1 Activity scheduling
This is one of the simplest interventions but also one of the most effective for depressed people. We have already illustrated how passivity and withdrawal are the two most typical safety behaviours practised by depressed individuals. Low energy levels, reduced motivation and exaggerated fears that they will make pretty poor company encourage such individuals to ‘hole up’ and do less and less. Often severely depressed people find it hard to do much more than lie in bed all day. Unfortunately, for reasons discussed above, giving in to the temptation of retreating and closing down is a policy that makes depressive symptoms worse.
Activity scheduling is a tool for combating passivity and gradually re-engaging the depressed person in some of the routines of his or her everyday life. At the same time it allows you to test out predictions based on depressive assumptions (‘I don’t enjoy anything these days…’; ‘I’m just a useless waste of space…’).
The first step in activity scheduling is simply to monitor one’s activity over a week by recording on a grid like the one below how you spend every hour. A brief entry is fine, but at the end of the hour make sure you also rate from 0 to 100 how bad your symptoms have been, i.e. how depressed you have felt during that hour. The benefits of doing this are twofold:
1. It allows you to take a baseline reading of your current activity levels. Often this can be a pleasant surprise in itself since many depressed people feel they achieve ‘absolutely nothing’ during the day (polarised thinking). Realising that they may have already been doing more than they think can start to break the cycle of paralysis. If activity levels have been severely restricted, at least you will be in a position to set realistic goals for yourself during the next phase.
2. By rating symptom intensity alongside your activities you will be able to work out the circumstances that make you feel more depressed and identify activities that take the edge off your symptoms. By analysing these patterns you can gradually introduce more of those activities that help you.
This is all very simple, obvious stuff but it introduces a level of objectivity and structure that you can very easily lose when the ‘black dog’ of depression threatens to take control.
Example of activity monitoring grid
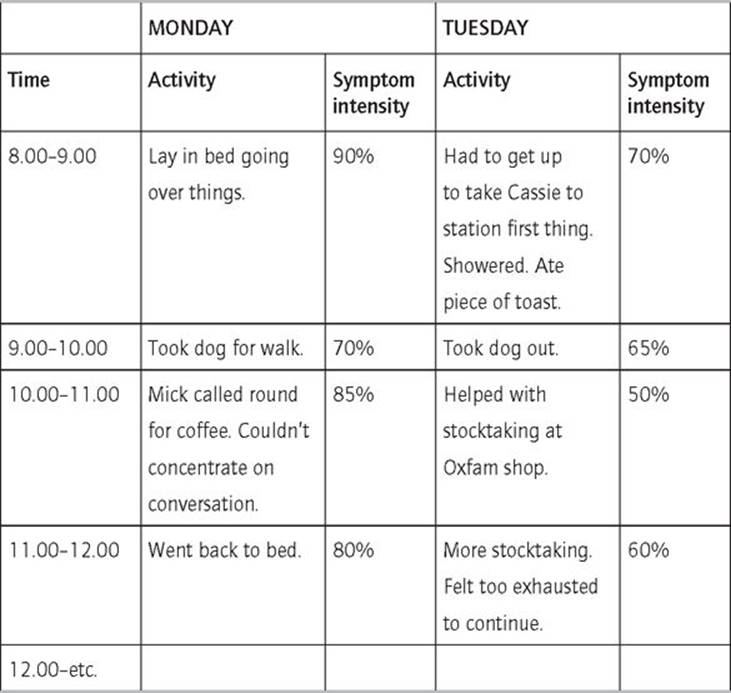
The next step
After you have done a week of recording, now is the time to use your knowledge to start pushing your activity levels up a little at a time. The key to doing this is to set realistic goals for yourself.
Rating how much you enjoy each of your planned activities (Pleasure rating: 0–100) and the sense of achievement it gives you (Mastery: 0–100) immediately afterwards will also help you confound your depressive expectations and start to help you feel less powerless. You can also use this information to schedule future activities likely to boost your mood.

The nature of depression is to feel overwhelmed. It is therefore really important not to be too ambitious in the targets that you set yourself - particularly in the early stages - and to make your goals very concrete and specific. If you bite off more than you can chew you will simply compound a sense of failure and strengthen the very thoughts and beliefs you are trying to weaken.
When you do start small be aware that your depression will tell you that what you are attempting is so modest that it won’t make any difference: ‘What does it matter if I get up at a regular time everyday? Big deal…’ However, as you master small, localised goals you will begin to build confidence for more ambitious projects. The whole process will gather momentum. As a famous oriental proverb states: ‘The journey of a thousand miles begins with a single step…’ Don’t let your depressive ‘all-or-nothing-thinking’ blind you to the truth of this.

Alex Johnson was a retired pilot who had become severely depressed following the death of his wife. Previously sociable and outgoing, Alex had become a virtual recluse, sitting at home and watching sport on the television day in, day out. This gave him ample opportunity to mull over how old and helpless he had become. As he cut himself off from his friends at the local rotary club Alex also lost confidence in his social skills. He kept telling himself that he was not ‘fit company’ at the moment and it would be far better if he waited until he was less depressed before he made any social overtures.
It was not easy to convince Alex that he was unlikely to feel better until he resumed the social activities that previously played such an important role in his life. His negative thoughts had convinced him that he was bound to embarrass himself and that everyone would notice how changed he was (catastrophising). In any case there seemed little point because, Alex insisted, he knew he would not enjoy himself.
In therapy Alex examined and started to consider the distorted assumptions that were keeping him secluded. How realistic were his fears? How obvious would the outward signs of his depression be to others?
After much gentle persuasion and some controlled ‘dry runs’ in the form of meals out with family members, Alex finally agreed to cross the threshold of his local club. He sensibly arranged for one of his friends to collect him and we agreed that he would stay for a minimum of half an hour.
In the event the other club members were delighted to see him, and Alex coped better than expected. He admitted that although he had been more subdued than usual he had nevertheless been ‘on surprisingly good form’. Certainly the anticipated public humiliation did not occur, and Alex confessed that ‘it had been good to see some familiar faces’.
Alex’s courage paid dividends. Building on this experience, over the next few months Alex started picking up the threads of his social life and frequented the club on a regular basis. The subsequent change in his demeanour and the accompanying reduction in his depressive symptoms were striking.
2 Using behavioural experiments to challenge depressive assumptions
Depressive assumptions and beliefs can usually be translated into testable predictions. This is well worth doing, even though your depressed mind might be telling you there is little to be gained and these kinds of experiment are largely pointless. The results will almost certainly emphasise the prejudicial nature of your depressive beliefs, as well as involving you in activities that are likely to increase your sense of mastery. Have a look at the chart below for an illustration of how your NATs and assumptions can provide the foundation for useful tests of your beliefs.
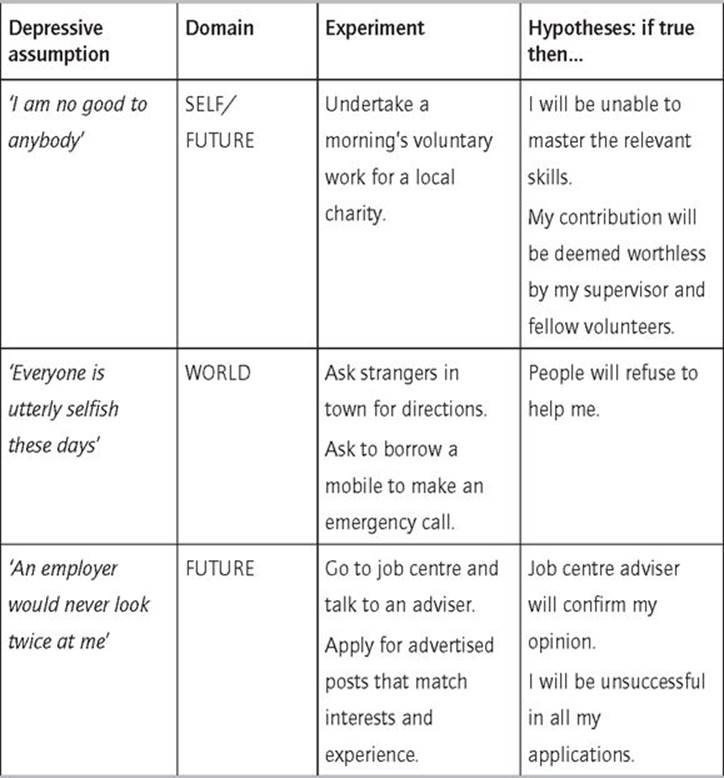
3 Exercise
Some studies suggest that regular aerobic exercise for 20 minutes three times a week is as effective in relieving depression as the most common antidepressants. The reason for this is that exercise releases more serotonin, the ‘feel good’ hormone into your body. Antidepressants also work by keeping your serotonin levels elevated and stopping the body reabsorbing them. Exercise is also good for your self-esteem. Not only does it give you the chance to see yourself achieving the manageable short-term goals you have set yourself as part of your fitness programme, but regular exercise boosts energy levels by making your body more efficient. You are also taking care of yourself, something that many depressed people find quite alien and, depending on which activity you pursue, sport may also encourage you to get out of the house and spend time with other people.
There are many, many forms of physical activity and even if you can’t picture yourself on the treadmill at the local gym you will almost certainly be able to find a form of exercise that suits you. Obviously, if you are new to exercise then do get the green light from your GP before you start your training for that marathon. If you suffer from depression, even if you have never tried exercise before, consider giving it a go. You might surprise yourself.